Melasma Treatment Guide for Patient-Focused Solutions and Clearer, Healthier Skin
Melasma treatment and management of facial pigmentation are critical skin care concerns that affect millions of people worldwide, often impacting confidence and quality of life. Whether you’ve just noticed uneven patches of skin pigmentation on face or have struggled with discoloration for years, seeking the right care is vital. In this comprehensive guide, we’ll explore what causes facial pigmentation and melasma, discuss the most effective facial pigmentation treatment options available today, and highlight how Dr. Stefan Weiss and the team at Trillium Dermatology deliver expert, compassionate care to help you achieve lasting results.
The Prevalence and Impact of Facial Pigmentation and Melasma
Facial pigmentation disorders, including melasma, are among the most frequent reasons patients seek dermatological advice. Melasma, in particular, is characterized by brown or gray-brown patches: most commonly appearing on the cheeks, forehead, upper lip, or chin, and represents one of the most challenging forms of facial pigmentation. While these conditions are not physically harmful, visible melasma symptoms can deeply affect emotional well-being, self-esteem, and social confidence.
Since facial pigmentation varies in severity and cause, personalized diagnosis and melasma treatment are essential. Unfortunately, one-size-fits-all solutions rarely deliver lasting improvement, especially for those seeking effective treatment for melasma on face, making expert guidance more important than ever.
Understanding Melasma and Facial Pigmentation: Causes, Risk Factors, Symptoms, and Diagnosis
Melasma and other types of facial pigmentation arise from a complex interplay of genetic, hormonal, and environmental factors. In melasma, pigment-producing cells (melanocytes) become overactive, leading to patchy discoloration and visible skin pigmentation on face. Common triggers include sun exposure, hormonal changes (such as pregnancy or birth control pills), genetic predisposition, and certain medications or cosmetic products.
Melasma symptoms and other facial pigmentation changes may range from small, faint spots to larger, more prominent patches. These changes are usually painless but can be persistent and challenging to treat without professional facial pigmentation treatment. Diagnosis typically involves a thorough skin examination, a review of medical history, and sometimes specialized imaging to determine the depth and pattern of pigmentation – an essential step in planning the most effective melasma treatment.
- Sun exposure: The leading trigger for pigmentation problems, as UV rays stimulate melanocyte activity and worsen melasma.
- Hormonal fluctuations: Pregnancy, hormone therapies, or birth control can precipitate melasma, sometimes called “the mask of pregnancy.”
- Genetics: A family history of pigmentation increases the risk of developing facial pigmentation.
- Skin type: Medium to darker skin tones are more prone to visible skin pigmentation on face and may require carefully tailored treatment for melasma on face.
Current Treatment Options for Melasma and Facial Pigmentation
Facial pigmentation or melasma treatment requires a customized plan, as no two cases are exactly alike. Board-certified dermatologists employ a comprehensive range of therapies, often in combination, to maximize facial pigmentation treatment results while minimizing side effects.
- Topical Therapies: Prescription creams containing ingredients like hydroquinone, tretinoin, azelaic acid, or kojic acid can lighten dark patches associated with melasma symptoms by inhibiting pigment production. These are often the first line of defense or treatment for melasma on face and may be used alone or in conjunction with other treatments.
- Chemical Peels: Supervised chemical exfoliation can help remove the outermost layers of skin, fading facial pigmentation, and stimulating healthier skin turnover. An experienced dermatologist carefully selects the chemical peel type and strength based on each patient’s skin type and sensitivity, and the depth of melasma involvement.
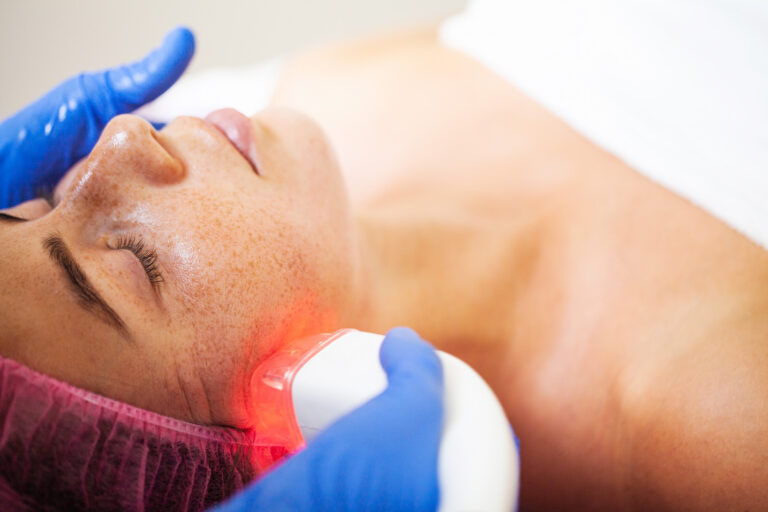
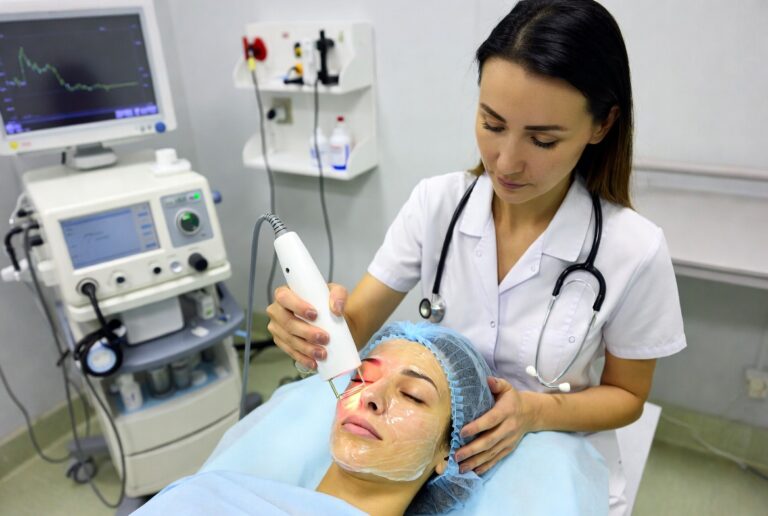
- Laser and Light-Based Treatments: Advanced devices such as fractional lasers and photofacials can target deeper pigmentation with precision, breaking up excess melanin while minimizing damage to surrounding tissue. Not all lasers are suitable for every skin tone, so expert assessment is crucial.
- Oral Medications: In select cases, oral medications such as tranexamic acid may be considered to help regulate pigment production, particularly for stubborn or recurrent melasma.
- Combination Approaches: Often, the best outcomes are achieved through a multimodal approach: integrating topical, procedural, and lifestyle modifications for comprehensive, lasting improvement in facial pigmentation.
Regardless of the chosen therapy, sun protection remains a cornerstone of melasma treatment and long-term management of facial pigmentation. Daily use of broad-spectrum sunscreen and physical barriers (like hats) is emphasized to prevent recurrence of melasma symptoms, protect treatment gains, and reduce ongoing skin pigmentation on face.
Emerging Therapies and Future Directions
The landscape of melasma treatment and facial pigmentation treatment is evolving rapidly. Researchers are investigating new topical agents that harness the skin’s microbiome to reduce inflammation and pigment production, as well as oral medications targeting underlying immune system pathways. Artificial intelligence and digital health tools are also being piloted to track melasma symptoms, predict flare-ups, and optimize treatment for melasma on face in real time.
Dr. Stefan Weiss stays at the forefront of these advancements by participating in clinical trials and integrating new, proven technologies as they become available. This commitment ensures patients at Trillium Dermatology always have access to the latest, most effective melasma treatment options, delivered with a focus on safety and individualized results for facial pigmentation concerns.
FAQs
Melasma symptoms typically include brown or gray-brown patches on the cheeks, forehead, upper lip, nose, or chin. The discoloration is usually symmetrical and may darken with sun exposure or hormonal changes.
No. While melasma is a form of facial pigmentation, it differs from sun spots or post-inflammatory hyperpigmentation in its triggers and behavior. Melasma is often hormonally influenced and tends to recur without ongoing management.
There is no single best treatment for melasma on face. Effective care usually involves a combination of topical therapies, sun protection, procedural treatments, and lifestyle adjustments. A personalized plan offers the best long-term outcomes.
Laser and light-based therapies can improve skin pigmentation on face, but melasma is a chronic condition. Procedures may reduce pigment significantly, but maintenance care and sun avoidance are essential to prevent recurrence.
Sun exposure is the primary trigger for melasma flare-ups. Without strict daily sunscreen use, even the best melasma treatment can fail. UV protection helps stabilize pigment production and preserves treatment results.
Conclusion
Living with facial pigmentation or melasma can be challenging, but expert, compassionate care makes all the difference. Dr. Stefan Weiss and the team at Trillium Dermatology combine deep expertise, advanced facial pigmentation treatment strategies, and a patient-first philosophy to help you achieve clearer, healthier skin. With a commitment to innovation, education, and support, you can trust that your melasma treatment journey will be guided by skilled hands and caring hearts.
If you’re ready to take control of your skin health and explore the latest solutions for facial pigmentation and melasma, schedule a consultation with Dr. Weiss at Trillium Dermatology. Discover firsthand how modern dermatology can restore your skin’s natural beauty and your confidence.