Table of Contents
What Is Psoriasis? (Medical Overview)
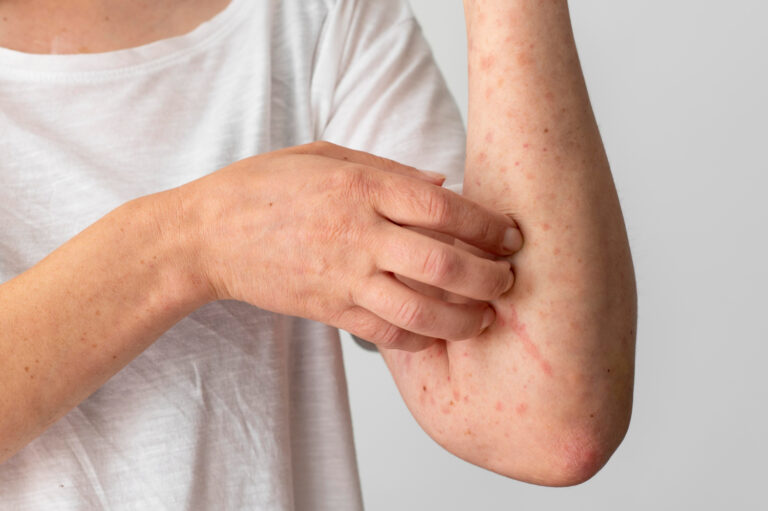
Latest psoriasis treatment discussions begin with understanding psoriasis itself, a chronic autoimmune skin disease that causes the immune system to mistakenly attack healthy skin cells. This immune dysfunction triggers an inflammatory response, resulting in red, scaly patches that can appear anywhere on the body. The hallmark symptoms include itching, burning, and discomfort, with periods of flare-ups (when symptoms worsen) and remission (when symptoms improve or disappear for a time). While psoriasis is not contagious, its visible signs can impact physical comfort and emotional well-being. Anyone can develop psoriasis skin condition, but it often emerges between the ages of 15 and 35 and tends to run in families.
Types of Psoriasis and Why Treatment Depends on the Type
There are several types of psoriasis, and understanding the specific type is crucial for determining the best treatment.
- Plaque Psoriasis: The most common form is plaque psoriasis, accounting for about 80-90% of cases. It’s characterized by raised, red patches covered with silvery scales, often found on the elbows, knees, scalp, and lower back.
- Scalp psoriasis: Scalp psoriasis causes flaking and scaling on the scalp, sometimes extending beyond the hairline.
- Guttate Psoriasis: Guttate psoriasis appears as small, drop-shaped lesions, typically after a bacterial infection like strep throat.
- Inverse Psoriasis: Inverse psoriasis affects skin folds, such as under the breasts or in the groin, and presents as smooth, red patches.
- Pustular Psoriasis: Pustular psoriasis is marked by white, pus-filled blisters and red skin, often on the hands and feet.
- Erythrodermic Psoriasis: Erythrodermic psoriasis is a rare, severe form that causes widespread redness and scaling, and can be life-threatening.
Each type responds differently to advanced psoriasis treatment approaches, including topical therapies, phototherapy for psoriasis treatment, and biologic treatment for psoriasis, making accurate diagnosis essential, especially within medical dermatology practices in regions such as North Carolina.
What Triggers Psoriasis Flare-Ups?
Psoriasis flare-up triggers can be unpredictable, but certain factors are known to trigger or worsen symptoms.
- Stress is a common culprit, as it can disrupt immune system balance.
Infections, such as strep throat or skin infections, may initiate or aggravate psoriasis, especially guttate psoriasis. - Weather changes, particularly cold, dry climates, can lead to drier skin and more frequent flares.
- Skin injuries (cuts, scrapes, or sunburns) can also provoke the Koebner phenomenon, where new lesions form at the site of injury.
- Certain medication classes, including lithium, beta-blockers, and antimalarial drugs, have been linked to flares.
- Lifestyle factors such as alcohol consumption and smoking are linked to increased disease severity.
Understanding how to prevent psoriasis flare-ups involves identifying personal triggers and addressing them through lifestyle modification, stress management, and dermatologist-guided care.
Psoriasis Treatment Goals (Set Expectations)
It’s important to understand that there is currently no cure for psoriasis. Even with new psoriasis treatment developments and psoriasis new treatment options, care focuses on controlling symptoms, reducing inflammation, and preventing flare-ups. Goals include minimizing visible lesions, relieving discomfort, preventing complications (such as psoriatic arthritis), and addressing emotional well-being.
Some patients achieve clear or nearly clear skin, while others may experience periodic flares. Realistic expectations, open communication with your dermatologist, and a personalized plan help ensure the best possible outcomes.
Topical Treatments for Psoriasis (Mild to Moderate Cases)
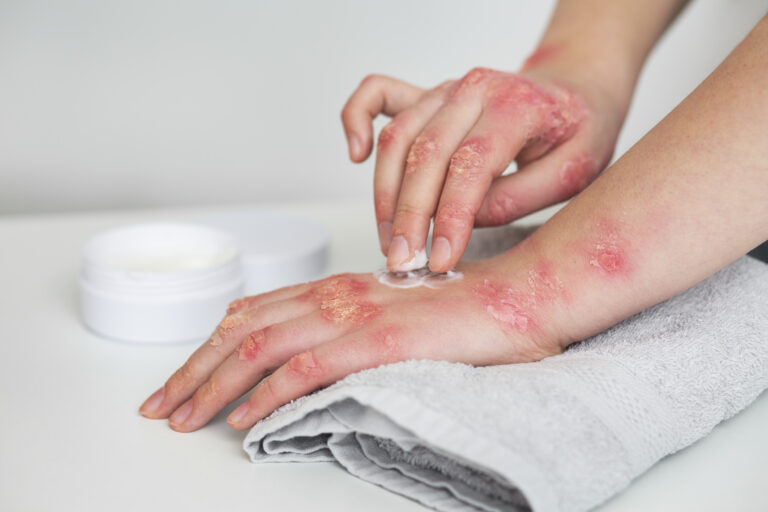
Topical therapies are usually the first line of treatment for mild to moderate psoriasis and remain a cornerstone of advanced psoriasis treatment strategies. Corticosteroid creams and ointments are the most frequently prescribed, as they quickly reduce inflammation, itching, and scaling associated with this psoriasis skin condition. Vitamin D analogs, such as calcipotriene, help slow skin cell growth and are often combined with steroids. Topical retinoids (like tazarotene) regulate cell turnover and reduce plaque formation. Coal tar and salicylic acid preparations can soften and remove scales. While over-the-counter options exist, it’s best to use all topical treatments under medical supervision to maximize benefits and minimize side effects like thinning skin or irritation.
Traditional Topical Therapies and Their Limitations
Corticosteroids and Vitamin D Analogs: For decades, topical corticosteroids and vitamin D analogues have been the mainstays of the best treatment approaches for psoriasis. These traditional topical therapies, though effective for many patients with this chronic autoimmune skin disease, often come with drawbacks such as skin thinning, irritation, or reduced efficacy over time. This has driven research into novel mechanisms and formulations, particularly for patients experiencing frequent psoriasis flare-up triggers.
New Non-Steroidal Topical Advances
The search for better, safer, and more tolerable treatments remains a priority for patients and clinicians alike. Recent advances in cutaneous immunology have resulted in new topical therapies or new psoriasis treatments, including Vtama and Zoryve, offering patients additional choices within psoriasis new treatments and renewed hope for effective management.
- Vtama (tapinarof) cream 1% is a first-in-class, non-steroidal topical medication approved by the FDA for the treatment of plaque psoriasis in adults. Unlike corticosteroids or vitamin D analogues, Vtama works as an aryl hydrocarbon receptor (AhR) agonist. This innovative mechanism targets inflammation and skin barrier dysfunction at the cellular level, helping to normalize skin cell growth and reduce the hallmark symptoms of psoriasis.
One of the key advantages of Vtama is its steroid-free formulation, which allows for long-term, continuous use without the risk of skin atrophy or tachyphylaxis (diminishing response over time). Clinical trials have demonstrated significant improvements in psoriasis severity scores, with many patients achieving clear or almost clear skin after just a few weeks of treatment. The cream is generally applied once daily to affected areas and is suitable for use on both the body and sensitive areas like the face and intertriginous zones – an important consideration when managing how to prevent psoriasis flare-ups.
In pivotal clinical studies, Vtama showed robust efficacy compared to placebo, with a favorable safety profile. Most side effects were mild to moderate and included folliculitis, contact dermatitis, and headache. Serious adverse events were rare. Importantly, Vtama does not carry the risks associated with long-term steroid use, making it particularly attractive for patients with chronic or widespread disease. Patients have reported high satisfaction rates, citing rapid improvement in lesions, minimal irritation, and the convenience of once-daily application.
- Zoryve (roflumilast) cream 0.3% is another groundbreaking, latest psoriasis treatment – topical therapy for plaque psoriasis. Approved by the FDA, Zoryve is a phosphodiesterase-4 (PDE4) inhibitor, a class of drugs that target a key enzyme involved in the inflammatory process. By inhibiting PDE4, Zoryve reduces the production of pro-inflammatory mediators, helping to control redness, scaling, and discomfort associated with psoriatic plaques.
Zoryve is applied once daily and is approved for use on all skin surfaces, including sensitive and intertriginous (skin fold) areas. Its non-steroidal, fragrance-free formulation is designed to minimize irritation and maximize tolerability – an important consideration for patients who require long-term, new psoriasis treatment strategies/management, including those receiving care in North Carolina dermatology practices.
Clinical trials of Zoryve have demonstrated promising results within psoriasis new treatment options. Patients treated with the cream experienced significant improvements in Psoriasis Area and Severity Index (PASI) scores, with many reporting complete or near-complete clearance of plaques associated with this psoriasis skin condition. The most common side effects were mild application site reactions, such as itching or pain, which generally resolved with continued use. Zoryve’s efficacy in sensitive areas, coupled with its favorable safety profile, makes it a valuable addition to the therapeutic arsenal for advanced psoriasis treatment.
Patient testimonials highlight the benefits of Zoryve’s gentle formulation, ease of use, and ability to maintain skin health without the concerns of steroid-related side effects. For individuals seeking alternatives to traditional topical therapies as part of a new psoriasis treatment strategy, Zoryve represents a significant advancement in personalized psoriasis care.
Both Vtama and Zoryve offer innovative, non-steroidal options for topical psoriasis management within the latest psoriasis treatment pathways. While Vtama targets the aryl hydrocarbon receptor and Zoryve inhibits PDE4, both work to reduce inflammation and restore the skin barrier in this chronic autoimmune skin disease. Their once-daily application, suitability for various body regions, and minimal risk of serious side effects set them apart from older treatments.
Importance Of Dermatologist Supervision
Choosing between Vtama and Zoryve may depend on patient preference, specific skin characteristics, medical history, and insurance coverage. Experienced dermatologists can tailor recommendations based on individual needs, helping patients manage psoriasis flare-up triggers and improve long-term outcomes. Both medications expand the options available, providing hope for those who previously struggled to find effective, tolerable topical therapies.
Phototherapy for Psoriasis (Light-Based Treatment)
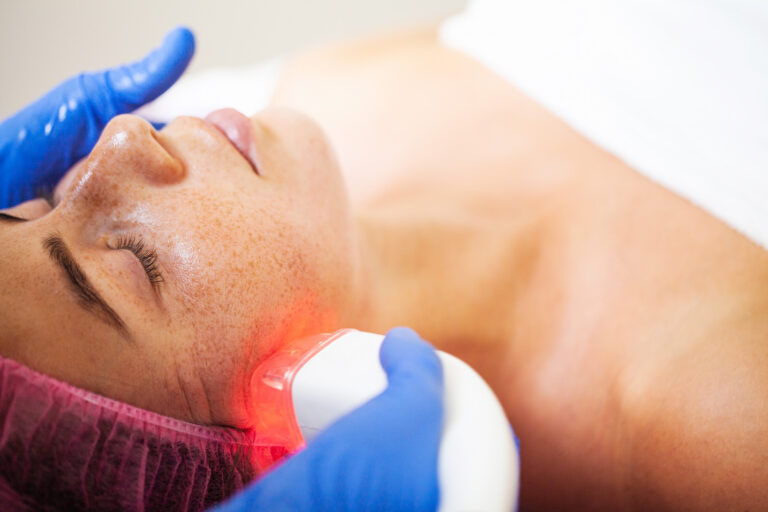
Phototherapy for psoriasis treatment, also known as light therapy, is an effective and well-established treatment for moderate psoriasis or when topical treatments haven’t worked. The most common form is narrowband ultraviolet B (NB-UVB) therapy, which involves exposing the skin to controlled amounts of UVB light in a medical setting. Treatments are usually given two to three times a week for several weeks. Phototherapy slows the rapid growth of skin cells and reduces inflammation associated with this psoriasis skin condition. It’s important to follow your dermatologist’s recommendations regarding frequency and duration, as overexposure can increase the risk of burns and skin cancer. Home phototherapy units are available in some cases, but these should always be used under medical guidance. Phototherapy is not suitable for everyone, and your dermatologist will determine if it’s right for you based on your type of psoriasis and health history.
Systemic Medications for Moderate to Severe Psoriasis
For patients with moderate to severe psoriasis or when other treatments have failed, systemic medications may be prescribed as part of advanced psoriasis treatment. These are taken orally or by injection and work throughout the body to suppress the immune response driving this chronic autoimmune skin disease.
- Methotrexate helps reduce inflammation and slow skin cell production, but requires regular blood tests to monitor for liver toxicity and other side effects.
- Cyclosporine is effective for rapid control of severe cases but is usually reserved for short-term use due to potential kidney and blood pressure risks.
- Oral retinoids (such as acitretin) normalize skin cell growth but can cause dryness and are not suitable for women who are pregnant or may become pregnant.
- Phosphodiesterase 4 (PDE4) inhibitors, like apremilast (Otzela), offer a targeted oral therapy with a different side effect profile.
Since systemic medications can have significant risks, ongoing monitoring and close dermatologist supervision are essential components of best treatment planning within medical dermatology practices, including those in North Carolina.
Biologic Treatments for Psoriasis (Advanced Care)
Latest psoriasis treatment advances include biologic drugs, which represent a major breakthrough in care for moderate to severe disease. These therapies are a cornerstone of advanced psoriasis treatment, particularly when topical or traditional systemic options fail.
Biologic drugs are made from living organisms and target specific parts of the immune system, such as tumor necrosis factor-alpha (TNF-alpha), interleukin-17, or interleukin-23, that drive inflammation in psoriasis. Biologics are administered by injection or intravenous infusion, and many can be self-injected at home after proper training.
Compared to older systemic drugs, biologics are often more effective and have a more targeted action, resulting in fewer side effects for many patients. However, they can increase the risk of infections and are not suitable for everyone. Your dermatologist will evaluate your medical history, lifestyle, and response to previous treatments before recommending a biologic treatment for psoriasis. Regular follow-ups are needed to monitor effectiveness and safety.
Examples of frequently prescribed biologic therapies include Bimzelex, Tremfya, Skyrizi, and Ilumya. These agents represent important psoriasis new treatment options, each offering distinct mechanisms of action and clinical benefits.
- Bimzelex, with the generic name bimekizumab, is a monoclonal antibody designed to inhibit both interleukin-17A (IL-17A) and interleukin-17F (IL-17F), which are cytokines implicated in the pathogenesis of the psoriasis skin condition. By targeting these two closely related cytokines, Bimzelex achieves robust suppression of the inflammatory pathways responsible for the development of psoriatic plaques. Clinical trials have demonstrated that Bimzelex can produce rapid and sustained clearance of skin lesions, with many patients achieving PASI 90 or PASI 100 responses (indicating 90% or 100% improvement in psoriasis severity indices) within a few months of this new psoriasis treatment.
Bimzelex is administered via subcutaneous injection, typically every four weeks after an initial loading phase. The safety profile of bimekizumab is generally favorable, though as with other IL-17 inhibitors, there is an increased risk of infections, particularly candidiasis (yeast infections), due to the role of IL-17 in mucocutaneous immune defense. Other potential adverse effects include upper respiratory tract infections, headache, and injection site reactions. Bimzelex is also being studied for other inflammatory conditions, such as psoriatic arthritis and ankylosing spondylitis, expanding its therapeutic potential in medical dermatology practice. - Tremfya, known generically as guselkumab, is a human monoclonal antibody that selectively targets interleukin-23 (IL-23), a key cytokine in the differentiation and maintenance of Th17 cells, which drive the inflammatory process in psoriasis. By inhibiting IL-23, Tremfya disrupts the signaling that promotes chronic skin inflammation and plaque formation and recurring psoriasis flare-up triggers. Approved for both moderate to severe plaque psoriasis and active psoriatic arthritis, Tremfya has shown high efficacy in clinical studies, with significant proportions of patients achieving clear or almost clear skin after several months of therapy.
Tremfya is administered as a subcutaneous injection, with an initial dose followed by a second dose four weeks later, and then maintenance doses every eight weeks. Its dosing schedule is less frequent than some other biologics, which may enhance convenience and adherence for patients.
Common side effects include upper respiratory infections, headache, and injection site reactions. Serious adverse events are rare, but as with all immunomodulatory therapies or medication, vigilance for infections and hypersensitivity reactions is necessary. Tremfya’s targeted mechanism allows for effective control of psoriasis with a generally favorable safety profile, reinforcing its role among the best treatment options currently available. - Skyrizi, or risankizumab, is another monoclonal antibody that works by inhibiting the p19 subunit of interleukin-23 (IL-23), similar to Tremfya, but with a distinct molecular structure. As part of the latest psoriasis treatment landscape, Skyrizi is approved for moderate to severe plaque psoriasis and, more recently, for active psoriatic arthritis. In pivotal clinical trials, Skyrizi has demonstrated substantial efficacy, with many patients achieving PASI 90 or PASI 100 responses and maintaining these improvements over long-term follow-up – outcomes that highlight the impact of new psoriasis treatment strategies in managing this chronic autoimmune skin disease.
The dosing regimen for Skyrizi involves subcutaneous injections every twelve weeks after two initial doses at week 0 and week 4, making it one of the most convenient biologic psoriasis new treatment options in terms of administration frequency.
The safety profile is similar to other IL-23 inhibitors, with upper respiratory infections, headache, and fatigue being the most commonly reported side effects. Skyrizi’s long dosing interval and strong efficacy make it a preferred option for patients seeking a highly effective and low-maintenance therapy. - Ilumya, with the generic name tildrakizumab, is also an anti-IL-23p19 monoclonal antibody, specifically designed for the treatment of moderate to severe plaque psoriasis. Among some of the advanced psoriasis treatments, Ilumya’s mechanism of action involves selective inhibition of the p19 subunit of IL-23, thereby blocking the downstream activation of Th17 cells and subsequent inflammatory cascades responsible for this psoriasis skin condition. Clinical studies have shown that Ilumya can provide significant improvement in skin clearance, with a high proportion of patients achieving PASI 75 or higher responses.
Ilumya is administered by subcutaneous injection every twelve weeks after two initial doses, aligning its dosing schedule with Skyrizi and making it suitable for patients who prefer infrequent injections. Its safety profile is consistent with other IL-23 inhibitors, with upper respiratory tract infections, injection site reactions, and diarrhea being the most common adverse events.
Rare but serious risks include hypersensitivity and increased susceptibility to infections. Although Ilumya has not been studied as extensively for psoriatic arthritis as Tremfya or Skyrizi, it remains a valuable biologic treatment for psoriasis in patients with skin-predominant disease.
Choosing Between IL-17 and IL-23 Biologics
While all four agents: Bimzelex, Tremfya, Skyrizi, and Ilumya, are highly effective for the treatment of moderate to severe plaque psoriasis, subtle differences exist in their mechanisms, dosing schedules, and clinical trial outcomes.
- IL-17 inhibitors like Bimzelex tend to produce a rapid onset of action and may be particularly effective for patients with severe, rapidly progressing disease.
- IL-23 inhibitors (Tremfya, Skyrizi, Ilumya) offer sustained efficacy and a lower frequency of dosing, which can improve patient adherence and convenience.
The choice among these therapies is often individualized, taking into account factors such as disease severity, history of psoriasis flare-up triggers, patient preference for dosing frequency, comorbid conditions (such as psoriatic arthritis), and risk profiles. The availability of multiple highly effective biologics has revolutionized psoriasis management, allowing many patients to achieve clear or almost clear skin and significantly improved quality of life.
Bimzelex, Tremfya, Skyrizi, and Ilumya represent the forefront of biologic treatment for psoriasis, offering targeted inhibition of key inflammatory pathways with proven efficacy and safety for this chronic autoimmune skin disease. As research continues and more real-world data become available, these agents are likely to play even greater roles in the personalized management of psoriasis and related inflammatory disorders. The expanding availability of psoriasis new treatment options allows patients and healthcare providers to now have an array of choices, enabling tailored treatment strategies that maximize outcomes and minimize disease burden.
Psoriasis Treatment by Location
Treatment approaches can differ depending on where psoriasis appears on the body.
- Scalp psoriasis may require medicated shampoos, topical steroids, or vitamin D analogs as part of an advanced psoriasis treatment strategy.
- Facial and inverse psoriasis (in skin folds) need gentle treatments, such as low-potency steroids or calcineurin inhibitors, to avoid irritation and thinning, especially important for this psoriasis skin condition.
- Nail psoriasis can be particularly stubborn, sometimes needing steroid injections, systemic therapies, or laser treatment as part of psoriasis new treatment options.
- Hand and foot psoriasis often requires a combination approach: topical treatments, phototherapy for psoriasis treatment, or systemic medication, because these areas are prone to painful cracks and fissures.
Since some locations are more sensitive or difficult to treat, working closely with a dermatologist trained in medical dermatology is vital.
Lifestyle Changes That Support Medical Psoriasis Treatment
Beyond medications, supportive lifestyle changes can improve your psoriasis outcomes and overall well-being when combined with the latest psoriasis treatment approaches.
- Moisturizing daily with fragrance-free creams helps prevent dryness and scaling.
Managing stress through techniques like yoga, meditation, or counseling can reduce psoriasis flare-up triggers. - A healthy diet rich in anti-inflammatory foods (fruits, vegetables, omega-3 fatty acids) may help some patients, though evidence is mixed.
- Another great method for preventing psoriasis flare-ups is to quit smoking and limit alcohol, which decreases its frequency and severity.
- Maintaining a healthy weight and being physically active support overall health and may improve the response to advanced psoriasis treatment.
- Always discuss any supplements or alternative therapies with your dermatologist to ensure they’re safe and effective for your situation.
When Should You See a Dermatologist for Psoriasis?
While mild cases of psoriasis can sometimes be managed with over-the-counter products, you should see a dermatologist if your symptoms are not improving, are getting worse, or are affecting your daily life. Expert evaluation is especially important when considering new psoriasis treatment options. Seek professional care if:
- Over-the-counter treatments fail to control your psoriasis skin condition
- Your skin develops pain, redness, swelling, or signs of infection
- You experience severe itching, bleeding, or widespread areas of involvement
- Psoriasis is impacting your mental or emotional health
- You notice joint pain, stiffness, or swelling (possible psoriatic arthritis)
Early intervention allows access to psoriasis new treatment options, including biologic treatment for psoriasis, and can prevent complications while improving long-term outcomes – particularly under specialist care in North Carolina.
What to Expect from a Dermatologist-Led Psoriasis Treatment Plan
Dermatologists create personalized treatment plans based on your type of psoriasis, severity, medical history, and lifestyle, aligning therapy with the best treatment approach for your disease. You may receive a combination of therapies (topical, phototherapy for psoriasis treatment, systemic medication, or treatment for psoriasis) tailored to your needs. Dermatologist-led care also includes regular follow-ups to monitor progress, adjust medications, and address side effects or new concerns. Your dermatologist will educate you about self-care, help identify psoriasis flare-up triggers, and coordinate with other specialists if you have related conditions (like psoriatic arthritis or depression). This comprehensive, patient-centered medical dermatology approach is designed for long-term disease control and quality of life improvement.
Psoriasis and Mental Health (Important but Often Missed)
Living with psoriasis can take a toll on your mental and emotional well-being. The visible nature of this chronic autoimmune skin disease may lead to self-consciousness, anxiety, or depression. Social situations, work, and relationships can be affected. It’s important to address these concerns openly; mental health is just as critical as physical health in advanced psoriasis treatment or care. Dermatologists can screen for emotional difficulties and refer you to counselors, support groups, or mental health professionals as needed. Treating both the skin and its psychological impacts leads to the best outcomes.
Emerging Biologic Pathways and Novel Targets
As our understanding of psoriasis pathogenesis grows, researchers are identifying new therapeutic targets that may shape the latest psoriasis treatment landscape. Agents that modulate the IL-36 pathway, tyrosine kinase inhibitors, and drugs affecting T-cell migration are in early-stage development. These innovations represent important psoriasis new treatment options for patients who do not respond to existing treatments or who experience intolerable side effects. The goal is to achieve better disease control with fewer adverse events, advancing psoriasis treatment strategies, and ultimately shifting care toward personalized medicine.
Why Choose a Board-Certified Dermatologist for Psoriasis Treatment
Choosing a board-certified dermatologist ensures you’re receiving care from a physician with specialized training and expertise in managing this psoriasis skin condition. Board certification indicates that the doctor has passed rigorous exams and stays updated on new psoriasis treatment research and treatment advances. Dermatologists are uniquely qualified to deliver advanced psoriasis treatment, prescribe biologic treatment for psoriasis, manage systemic medication, recognize potential side effects early, and tailor treatments to your individual needs. Their experience with complex cases within medical dermatology ensures safer, more effective care and better long-term results – especially important for patients receiving specialty care in North Carolina.
Frequently Asked Questions (FAQs)
No, psoriasis is not contagious. You cannot catch this chronic autoimmune skin disease from anyone or transmit it to someone else.
While no specific diet cures psoriasis, maintaining a healthy weight and eating anti-inflammatory foods may help reduce psoriasis flare-up triggers for some people.
Response times vary depending on the best treatment selected. Some treatments work within weeks, while others may take several months. Consistency and patience are key.
Psoriasis can be associated with other health issues, such as psoriatic arthritis, heart disease, and depression. Regular check-ups with your dermatologist help monitor risks and optimize advanced psoriasis treatment.
Biologic treatment for psoriasis is generally safe when used under a dermatologist’s supervision, but it can increase the risk of infections. Your doctor will weigh the benefits and risks for your situation.
Psoriasis usually requires long-term management, even if your skin becomes clear. Stopping treatment without guidance may cause flares.
Look for a board-certified dermatologist, which you can verify at the American Academy of Dermatology website or by asking your primary care provider for a referral.
Conclusion
Psoriasis is a complex and often challenging condition, but today’s treatment options can significantly improve symptoms and quality of life. From topical therapies and phototherapy for psoriasis treatment to advanced systemic and biologic treatment for psoriasis, there are effective solutions for nearly every patient. Addressing lifestyle factors, mental health, and psoriasis flare-up triggers further strengthens outcomes. If your psoriasis is persistent, worsening, or impacting your daily life, don’t hesitate to consult a board-certified dermatologist. By scheduling an appointment with board-certified dermatologists, you can get expert guidance and personalized psoriasis new treatment options, for better control over your condition and for a comfortable and confident life.