Topical steroid - A Guide to Safe Use and Awareness of Potential Risks
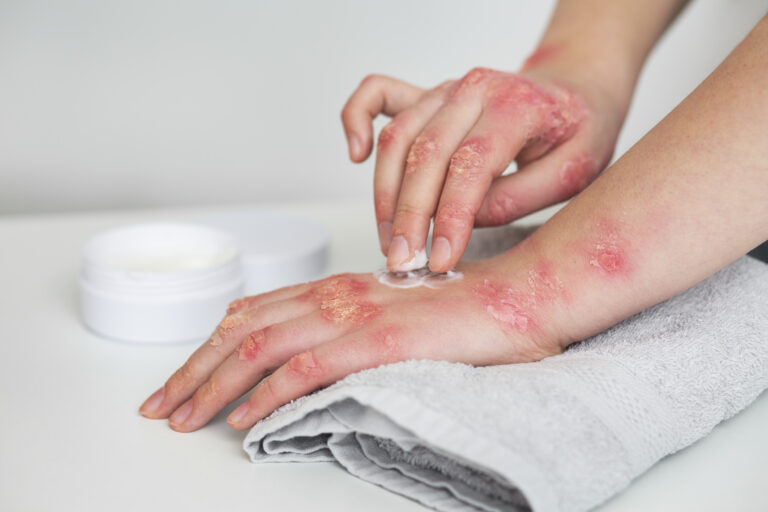
Topical steroids are powerful and effective medications widely used to treat a variety of inflammatory skin conditions, such as eczema, psoriasis, dermatitis, and allergies. For millions, these creams and ointments offer relief from itching, redness, and discomfort, restoring confidence and quality of life. However, as with all medicines, their benefits are balanced by potential risks, especially when misused or overused. An increasing number of individuals and healthcare professionals are raising awareness of topical steroid side effects and the complex phenomenon known as topical steroid withdrawal (TSW).
In this article, we’ll explore what topical steroids are, the side effects you should know about, the realities of topical steroid withdrawal, and how to use these medications safely and responsibly.
What Are Topical Steroids?
Topical steroids (also called topical corticosteroids) are medications applied directly to the skin to reduce inflammation and suppress immune responses. They come in various strengths, from mild (such as hydrocortisone 1%) to very potent (such as clobetasol propionate). Physicians may prescribe these drugs for short- or long-term use, depending on the condition being treated.
Common Side Effects of Topical Steroids
When used as directed and for short periods, topical steroids are generally safe and effective. However, prolonged or inappropriate use can lead to a spectrum of unwanted side effects. Understanding these risks helps promote safe and informed treatment decisions.
Skin Thinning (Atrophy)
One of the most common topical steroid side effects is skin thinning. Over time, steroids can break down collagen, making the skin appear translucent, fragile, and more susceptible to bruising or tearing. This is particularly concerning on parts of the body where the skin is already thin such as the face, underarms, or groin.
Stretch Marks (Striae)
Strong topical steroids, especially if used improperly or on large areas, can cause stretch marks. These are permanent lines that appear when the skin’s underlying support structure is weakened.
Perioral Dermatitis and Acne
Topical steroid side effects can include triggering or worsening perioral dermatitis – a rash around the mouth or causing steroid-induced acne. These eruptions often appear as small red bumps or pustules, especially with repeated or high-potency use.
Changes in Skin Color (Hypopigmentation or Hyperpigmentation)
Steroids can sometimes lighten or darken the skin in treated areas. This effect can be particularly distressing for individuals with deeper skin tones.
Increased Hair Growth (Hypertrichosis)
Some individuals may notice increased fine hair growth in areas where topical steroids are applied frequently.
Delayed Wound Healing
Since corticosteroids suppress immune activity, healing of cuts, scrapes, or wounds may be slower in affected areas.
Systemic Absorption and Rare Effects
Although rare, topical steroids, especially strong ones used over large surface areas or under occlusion (bandages) can be absorbed into the bloodstream and cause systemic side effects. These may include hormonal imbalances, suppression of adrenal gland function, and even growth retardation in children.
Topical Steroid Withdrawal (TSW): A Growing Concern
In recent years, patient advocacy groups and dermatologists have brought attention to topical steroid withdrawal, also known as “red skin syndrome.” TSW is a constellation of symptoms that can occur after discontinuing topical steroids, particularly following prolonged or inappropriate use. While the phenomenon is still under active research, it is increasingly recognized in medical literature.
What Causes TSW?
Topical steroid withdrawal is thought to result from the skin and body adapting to the presence of topical steroids. When the medication is stopped suddenly, the skin can react dramatically, leading to a rebound in inflammation and other symptoms.
Symptoms of Topical Steroid Withdrawal
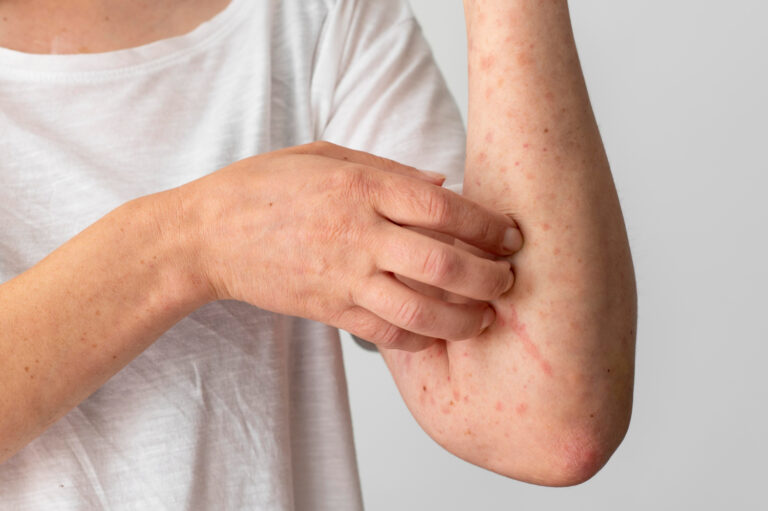
- Red, burning, or stinging skin that may spread beyond the original area of application
- Intense itching and discomfort
- Swelling, oozing, or crusting lesions
- Dry, flaky, or peeling skin
- Insomnia and mood changes due to physical discomfort
These symptoms may persist for weeks or even months, and can significantly impact a person’s quality of life. Recognizing these symptoms early is essential to managing topical steroid side effects and withdrawal effectively.
Who Is at Risk?
Individuals who have used moderate to high-potency topical steroids for extended periods, especially on sensitive skin areas or under occlusion, are at greatest risk for TSW. Children and those with chronic skin conditions may be particularly vulnerable.
Safe Use and Prevention
The good news is that, for most people, topical steroids are safe when used properly and under medical guidance. Here are some tips to minimize the risk of topical steroid side effects and withdrawal:
- Follow your healthcare provider’s directions carefully, only use the prescribed amount, frequency, and duration.
- Avoid long-term or continuous use unless explicitly advised by your doctor.
- Use the lowest effective potency for the shortest duration needed to control symptoms.
- Do not apply steroids to broken skin, large areas, or under bandages unless instructed.
- If you are concerned about side effects, topical steroid withdrawal, or need to stop treatment, consult with your healthcare provider. They may recommend gradual tapering rather than abrupt discontinuation.
- Monitor your skin for any signs of thinning, color changes, or unusual reactions, and report these to your doctor.
Conclusion
Topical steroids are powerful allies in the management of many skin conditions, but their use requires caution and respect. Awareness of potential topical steroid side effects and the reality of topical steroid withdrawal empowers patients to seek guidance, monitor for adverse effects, and use these medications as part of a broader, holistic approach to skin health. Your skin’s safety and your peace of mind are worth it. For this, make sure you consult an experienced dermatologist.